EHR software development is the process of designing, building, and deploying electronic health record systems that store, manage, and exchange patient health information across healthcare organizations. EMR software development focuses on similar capabilities but typically within a single practice or organization. Both require deep integration with clinical workflows, regulatory compliance (HIPAA, GDPR, PDPA), and interoperability standards like HL7 FHIR.
If you’re evaluating EHR software development or EMR software development, treat it as a clinical workflow + regulatory + interoperability program, not “just another SaaS build.” The global electronic health record market is projected to reach USD 47.97 billion by 2032, growing at roughly 11% CAGR, which means the pressure to build or modernize EHR systems is only increasing.
Most EHR development failures come from (1) unclear clinical workflows, (2) under-scoped integrations, (3) weak data governance, (4) usability debt, and (5) compliance handled too late.
What I’d do in your position:
1) Map 3–5 highest-impact workflows end-to-end, 2) agree on a minimum interoperable data set (FHIR resources + vocabularies), 3) define a security/compliance baseline early (HIPAA/GDPR/PDPA/APPs), 4) run a thin-slice prototype through real clinicians, and 5) choose build vs buy using a total cost of ownership (TCO) model.
Key takeaways for EHR and EMR software development
- EHR vs EMR: EHR is designed for broader interoperability and continuity of care; EMR is often more “within one organization.” (Vendors vary, so define it in your requirements.)
- Interoperability is not optional: Build around HL7 FHIR and plan for SMART on FHIR if you need app extensibility and modern authorization patterns.
- Compliance is design input, not a checklist: HIPAA Security Rule expects administrative/physical/technical safeguards; NIST provides practical guidance to implement them.
- Usability drives adoption and safety: Poor UI increases documentation time, workarounds, and clinician burnout. Budget for user research and usability testing.
- Build vs buy is usually “hybrid”: Many organizations buy a certified core and build differentiating workflows, patient portals, and analytics on top via APIs.
- Market context: The electronic health record market continues to expand, driven by digitization mandates and value-based care. If you invest in EHR development now, you avoid the significantly higher cost of retrofitting interoperability and compliance later.
Introduction: Why EHR Software Development Matters Today
What EHR software is (plain definition): An Electronic Health Record (EHR) system is software that stores, manages, and exchanges patient health information to support clinical care, operations, compliance, and reporting across a healthcare organization, and increasingly, across organizations. If you plan to build an EHR system, understanding this scope is essential before writing a single line of code.
Why custom EHR development differs from off-the-shelf: Off-the-shelf EHRs optimize for broad market fit and compliance; custom EHR software development for a specific organization optimizes for your workflows, integrations, and strategic differentiation. That’s valuable, but it also transfers more responsibility to you (security, regulatory compliance, uptime, and change management). The same applies to EMR software development, especially if your scope is a single practice or specialty.
Who this guide is for:
- Healthcare providers modernizing legacy systems
- Digital health startups building vertical EHRs
- Enterprises integrating EHR/EMR modules into platforms
- Procurement teams comparing vendors vs custom builds
- Organizations evaluating an EHR software development company or EMR software developers
What you’ll learn:
How EHR development and EMR software development decisions affect cost, timelines, clinical efficiency, interoperability, and long-term operational flexibility. You’ll also get a practical development process, stack guidance, and a decision checklist, useful whether you’re building in-house or working with an EHR software development company.
What Is EHR Software? (Foundational Understanding)
What is the difference between EHR and EMR?
An EMR (Electronic Medical Record) is a digital version of a patient chart used within a single practice or organization. An EHR (Electronic Health Record) is designed for broader sharing and interoperability across labs, imaging centers, pharmacies, and other providers, with a stronger emphasis on continuity of care. The key difference: EHR systems exchange data across organizations, while EMR systems typically stay within one.
In practice, vendors use the terms loosely. The better approach: define scope by use cases and interoperability requirements, not marketing labels. The distinction matters for architecture: electronic health record software designed for multi-provider data exchange needs different integration patterns than a single-practice EMR.
The core purpose of EHR systems
A modern EHR supports:
- Clinical care delivery (documentation, orders, results, e-prescribing, clinical decision support)
- Operational efficiency (scheduling, revenue cycle management, utilization reporting)
- Regulatory compliance (privacy, audit trails, retention, breach handling)
- Interoperability (exchanging data using standards like HL7 FHIR)
How EHRs support workflows
EHRs sit at the center of:
- Clinical workflows: triage → encounter → orders → results → follow-up
- Administrative workflows: registration → eligibility → billing → claims
- Regulatory workflows: access controls, audit trails, breach notification processes
Common misconceptions (that derail projects)
- “We can bolt interoperability on later.” Usually false; data models and integration architecture patterns should be designed early.
- “Clinicians will adapt.” They will, by creating workarounds that harm data quality and safety.
- “Compliance is a final QA step.” Compliance requirements shape architecture, logging, encryption, and access control from day one.
Explore Our Healthcare Software Development Services
How does EHR software improve clinical workflows?
This is where EHR software development and EMR software development create real ROI, by removing friction from workflows that clinicians repeat dozens or hundreds of times a day. A well-designed EHR can reduce documentation time by 30–50%, cut duplicate lab orders, and improve billing accuracy. A poorly designed one does the opposite: it adds clicks, creates workarounds, and burns out the people it was supposed to help.
The clinical workflow problems EHRs can solve (and how)
Problem A: Documentation takes too long
- Fix: reduce user interface complexity, use templates intelligently, automate structured data capture, and integrate voice recognition carefully (with review workflow).
- Pitfall: over-templating creates “note bloat” and can increase medical error risk.
Problem B: Orders/results are fragmented across systems
- Fix: integration development with labs/imaging/pharmacy, unified inbox/tasking, and status tracking.
- Pitfall: “best-effort” interfaces without reconciliation logic create missing results and duplicate orders.
Problem C: Care teams can’t see the same truth
- Fix: role-based, team-based views; consistent patient identity; problem list governance; data ownership rules.
Problem D: Patients are stuck outside the loop
- Fix: patient portals, patient management portal features (appointments, results, messaging), and clear consent flows to improve patient satisfaction.
Practical “thin-slice” example (what I’d do)
If you’re unsure where to start with EMR software development, pick one end-to-end “thin slice,” such as:
New patient intake → visit note → lab order → result review → patient message → billing handoff
Build/prototype this slice first. It forces stakeholder requirements gathering, integration requirements, and security requirements into one contained scope before you scale.
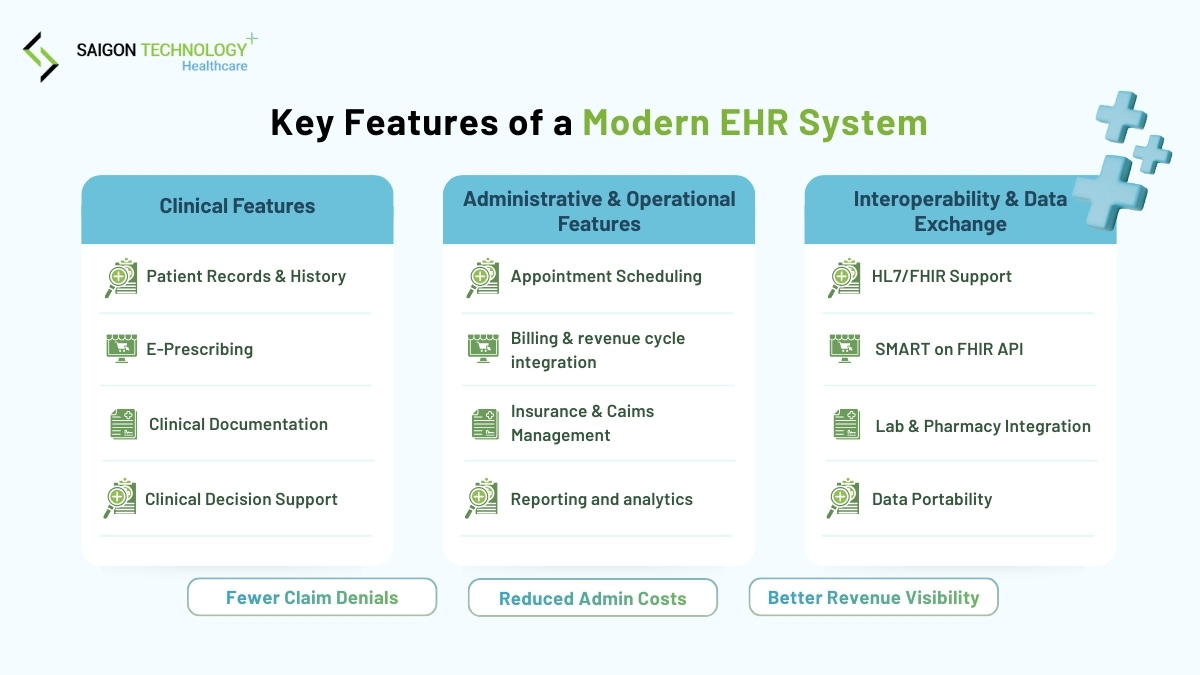
What are the key features of a modern EHR system?
Below are the core features most decision-makers expect in EHR software development companies’ proposals. Use these as a requirements baseline, then add your unique workflows.
1. Clinical features
- Patient records & medical history: problems, meds, allergies, immunizations, encounters
- Clinical documentation & charting: notes, structured forms, templates, attachments
- E-prescribing: medication selection, safety checks, refill workflows (country-specific)
- Clinical decision support (CDS): alerts, reminders, guideline prompts, risk scores (with careful governance)
Regulatory note (US): CDS can intersect with FDA oversight depending on functionality and intended use; understand how your CDS features are categorized.
2. Administrative & operational features
- Appointment scheduling: multi-location, provider templates, reminders
- Billing & revenue cycle integration: coding support, claim generation, payment posting, denial workflows
- Insurance and claims management: eligibility checks and payer interfaces vary by region
- Reporting and analytics: quality reporting, operational efficiency dashboards, throughput
Where you often see real ROI:
- Billing accuracy improvements (fewer denials, cleaner claims)
- Administrative cost savings through automated eligibility, reduced rework
- Better revenue cycle management visibility (aging, denial reasons)
3. Interoperability & data exchange
Interoperability should be explicit in your EHR development scope:
- HL7 / FHIR support: FHIR is a widely used API-focused standard for exchanging healthcare information.
- SMART on FHIR: adds a secure app integration layer using open standards like OAuth2 and OpenID Connect.
- Integration with labs, imaging, pharmacies, and devices: plan for interface monitoring, retries, reconciliation, and downtime behavior
- Data portability: export and patient access patterns; consider Bulk Data where relevant (population health, analytics)
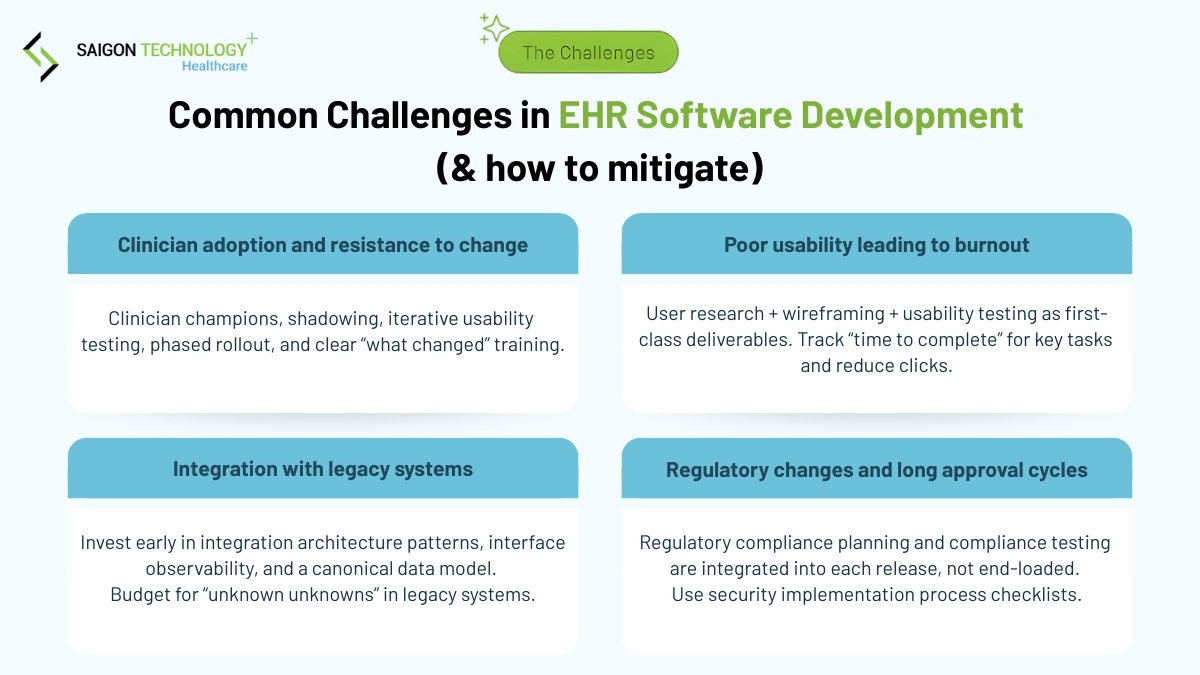
Common challenges in EHR and EMR software development (and how to mitigate)
These are the failure modes I see most often, whether you’re building a full electronic health record system or a focused EMR for a single specialty.
1. Clinician adoption and resistance to change
According to the Office of the National Coordinator for Health IT (ONC), approximately 96% of non-federal acute care hospitals and 78% of office-based physicians now use certified EHR systems. However, adoption does not equal satisfaction. A Mayo Clinic study found that clinician burnout is strongly associated with EHR usability, and poor EHR design remains one of the top drivers of physician dissatisfaction.
Mitigation: clinician champions, shadowing, iterative usability testing, phased rollout, and clear “what changed” training.
2. Poor usability leading to burnout
Mitigation: treat user research, wireframing, and usability testing as first-class deliverables, not afterthoughts. Track “time to complete” for key tasks and actively reduce click counts.
3. Integration with legacy systems
Mitigation: invest early in integration architecture patterns, interface observability, and a canonical data model. Budget for “unknown unknowns” in legacy systems.
4. Regulatory changes and long approval cycles
Mitigation: regulatory compliance planning and compliance testing integrated into each release, not end-loaded. Use security implementation process checklists.
Compliance, Security, and Privacy Requirements
Compliance failures are expensive. HIPAA penalties range from $100 to $50,000 per violation (up to $1.5 million per year per category), and a single data breach can cost healthcare organizations an average of $10.93 million, according to IBM’s 2023 Cost of a Data Breach Report. That makes compliance a business-critical design input, not a box to check at the end.
1. U.S. compliance (HIPAA)
According to the U.S. Department of Health and Human Services, the HIPAA Security Rule requires “reasonable and appropriate” administrative, physical, and technical safeguards for protecting electronic protected health information (ePHI). For practical implementation, NIST SP 800-66 Rev. 2 maps specific security program activities to HIPAA requirements and is widely used as the de facto implementation guide by EHR development teams.
What to build into your EHR from day one:
- Access controls (role-based access controls, least privilege)
- Audit trails (who accessed what, when, from where, what changed)
- Data encryption (at rest and in transit)
- Breach notification procedures readiness (logs, incident response playbooks)
2. Global & regional considerations (EU, Singapore, AU)
- EU (GDPR): health data is treated as a special category; you need a valid legal basis/condition and strong safeguards.
- Singapore (PDPA): PDPA sets obligations for collection, use, disclosure, and care of personal data; PDPC provides healthcare sector guidance, including transfer limitation and breach notification obligations.
- Australia (APPs): the Australian Privacy Principles are the cornerstone framework under the Privacy Act 1988, governing how covered entities handle personal information (including health information guidance).
Practical guidance: If you operate across regions, design around the strictest common controls: data minimization, explicit access control, auditability, retention policies, and cross-border transfer controls. At Saigon Technology, our ISO 27001-certified security processes and experience delivering HIPAA-compliant healthcare software across the US, Australia, Europe, and Singapore mean these controls are built into our EHR development workflows from day one, not added as an afterthought.
3. Security best practices (applied, not abstract)
For EHR software development company evaluations, ask whether they can operationalize these:
- RBAC + MFA (multi-factor authentication): enforce MFA for privileged access; review roles quarterly
- Segmentation of environments: separate prod/non-prod; never use real patient data in test unless you have a formal process
- Threat modeling and secure SDLC: require code review, dependency scanning, and penetration testing
- Security verification standard: OWASP ASVS provides a concrete checklist of web application security controls and test requirements.
- Disaster recovery: define RPO/RTO targets and run restore tests (not just backups)
Interoperability Standards and Data Governance
Why interoperability affects outcomes and cost
Interoperability reduces duplicate testing, supports continuity of care, and enables safer coordination, but only if data quality and governance are enforced. For EHR developers and EMR software developers, this is where architecture decisions made early either pay dividends or create years of technical debt.
What interoperability standards should EHR systems support?
According to HL7 International, FHIR (Fast Healthcare Interoperability Resources) is the leading standard for exchanging healthcare information electronically using modern RESTful APIs. Here are the three standards most relevant to EHR software development:
- HL7 FHIR: the primary standard for healthcare data exchange via APIs. FHIR uses resources (Patient, Observation, Medication, etc.) that map to clinical concepts, making integration development faster and more predictable than older standards.
- SMART on FHIR: according to SMART Health IT, this is a standards-based framework that lets third-party apps securely integrate with EHRs using OAuth2 and OpenID Connect for authorization.
- HL7 CDA: a document markup standard for clinical document exchange (still relevant in many ecosystems, especially for Continuity of Care Documents).
Real-world use cases for FHIR-based APIs
- Patient-facing apps accessing records (with proper consent)
- Provider-to-provider exchange and referral workflows
- Population health management and predictive analytics pipelines
- Device and IoT device integration (where appropriate governance exists)
Data governance (the “unsexy” part that saves projects)
Define:
- Data ownership: who owns problem list, meds, allergies, demographics
- Data quality rules: required fields, code systems, validation checks
- Access control model: data access control by role, location, encounter, and sensitivity
- Retention and deletion: align with regulatory requirements by region
Avoiding vendor lock-in:
Lock-in often happens at the data model + integration layer. The best defense is:
1) enforce API-first patterns (FHIR where feasible), 2) maintain an internal canonical model for analytics, and 3) ensure you can export data in a usable format.
Custom EHR Development vs Ready-Made Solutions
This is where most executive teams need decision support; the choice between custom EHR software development, an off-the-shelf EMR, or a hybrid approach has long-term cost, compliance, and operational implications.
1. When custom EHR or EMR software development makes sense
Custom EHR software development or EMR software development is usually justified when you have:
- Specialized clinical workflows (e.g., oncology protocols, complex multi-disciplinary pathways)
- Differentiation needs (unique patient experience, proprietary care models)
- Integration complexity (many legacy systems + custom processes)
- A long runway where operational flexibility matters more than speed
2. Pros and cons comparison (build vs buy vs hybrid)
| Option | Best for | Strengths | Trade-offs/risks |
| Buy a ready-made EHR/EMR | Standard workflows, faster go-live | Known feature set, vendor support, sometimes certification-ready | Customization limits, licensing fees, integration constraints, vendor roadmap risk |
| Build custom (full) | Unique workflows, platform differentiation | Full control, tailored UX, flexible integrations | Higher implementation risk, longer timelines, must own compliance/security and ongoing operational costs |
| Hybrid (common) | Most mid-to-large orgs | Buy core + build modules (patient portal, analytics, specialty workflows) | Requires strong integration architecture patterns and governance to avoid “two EHRs” experience |
What I’d do in your position:
If you’re in the US and need regulatory alignment with certified ecosystems, I’d seriously consider a hybrid approach and validate interoperability requirements early (FHIR + SMART where relevant). For US programs that interact with certified EHR technology, note how the Promoting Interoperability programs emphasize interoperability and use of certified EHR tech.
Context on major EHR platforms: Epic, Oracle Health (formerly Cerner), MEDITECH, and Allscripts dominate the US hospital market. If you’re building custom modules or integrations around these platforms, your EHR software development scope shifts toward API-based extensions (often via FHIR), custom workflows, patient portals, and analytics, not replacing the core. For smaller practices, open-source options like OpenMRS or proprietary SaaS EHRs may serve as a foundation for EMR software development with custom modules on top.
What is the best technology stack for EHR software development?
There’s no single “best” stack for EHR software development or EMR software development, but there are predictable requirements: auditability, security, scalability, integration performance metrics, and maintainability.
A practical reference architecture
- Frontend: React (Next.js), Angular 16+, or Vue 3 with strict accessibility (WCAG 2.1) and component governance. For clinician-facing dashboards, prioritize fast rendering and offline-capable design.
- Backend: .NET Core/ASP.NET 6+, Node.js (Express), Java 18/Spring Boot, or Python (FastAPI, Django). Use modular services with strong domain boundaries — not necessarily microservices on day one.
- Database systems: PostgreSQL or SQL Server for transactional integrity; consider a separate analytics store (e.g., ClickHouse, BigQuery) for reporting workloads.
- Search: Elasticsearch or OpenSearch for chart search and document retrieval (with strict access controls on PHI).
- Integration layer: API gateway + FHIR server (e.g., HAPI FHIR, Azure Health Data Services) + message/eventing (Apache Kafka, RabbitMQ) where needed; interface engine for HL7 v2 where relevant.
- Identity & access: OAuth 2.1, SAML/OpenID Connect, MFA, RBAC, and centralized audit logging. Consider HashiCorp Vault or AWS Secrets Manager for secrets management.
- Cloud infrastructure: AWS, Microsoft Azure, or Google Cloud, choose based on regional hosting, compliance certifications (HIPAA BAA, SOC 2), and vendor support. Hybrid approaches if data residency requires on-premise components.
- Mobile: React Native, Flutter, or native (Kotlin/Swift) for clinician-facing mobile apps, with offline-first patterns for areas with poor connectivity.
Stack selection criteria (what procurement should ask)
- Can you support system downtime gracefully (read-only mode?, queued orders?)
- How do you isolate tenants and sensitive workflows?
- How do you handle data migration and data validation at scale?
- What is your approach to testing and quality assurance, including security and usability testing?
- What’s the plan for annual maintenance and support costs?
EHR Software Development Process (Step-by-Step)
This process applies to in-house EHR developer teams and outsourced EMR software developers alike.
1. Discovery & requirements analysis
Do stakeholder requirements gathering with:
- Clinicians (different specialties, nurses, allied health)
- Admin staff (front desk, billing, medical records)
- IT/security/compliance
- Finance/procurement (cost constraints, vendor requirements)
Deliverables that reduce risk:
- Workflow maps (current vs future)
- Market research and feasibility analysis (what must be integrated, what can change)
- Data governance decisions and regulatory compliance planning
2. UX/UI design for clinicians
Non-negotiables:
- User research: shadowing, contextual inquiry
- Wireframing + prototyping: test with real scenarios
- Usability testing: measure task completion time and error rates
- Accessibility and responsive design (clinics, wards, tablets)
3. Architecture & technology decisions
Decide early:
- Cloud vs on-premise vs hybrid (data residency, latency, operational maturity)
- Integration architecture patterns (sync vs async, retries, idempotency)
- Scalability planning (peak hours, batch jobs, reporting)
4. Development & testing
A healthcare-appropriate QA strategy includes:
- Functional tests for critical flows (meds, allergies, orders)
- Security testing (penetration, dependency, config)
- Performance testing (peak clinic hour)
- Compliance testing (audit trails, access controls)
- Validation and UAT with clinicians (realistic scripts)
5. Deployment & maintenance
Plan for:
- Deployment planning and preparation (cutover checklists, rollback plans)
- Go live support and monitoring (war rooms, incident triage)
- Data migration (reconciliation reports, clinician sign-off)
- Ongoing updates with documented change management
Real-world example: Saigon Technology’s healthcare team built AxiaGram, a US-based medical records platform managing 6 million+ medical records, reducing development time by 40% through a dedicated offshore team model. In another engagement, a telehealth platform scaled to handle 50,000+ patient interactions per month using a HIPAA-compliant architecture with HL7 FHIR integration. These outcomes required the full process above: discovery through deployment, with compliance and clinical validation at every stage.
Best Practices for Successful EHR and EMR Software Development (and cost/timeline reality)
Best practices
- Clinician-first design (optimize for clinical efficiency, not admin convenience)
- Incremental rollout with feedback loops
- Observability built-in (integration monitoring, audit trails, uptime metrics)
- Security requirements embedded from sprint 1 (HIPAA/GDPR/PDPA/APPs)
- Strong documentation and training to support user adoption from day one
- Choose an EHR software development company with proven healthcare delivery experience, compliance certifications (ISO 27001, ISO 9001), and a track record of managing sensitive patient data at scale
Cost and timeline expectations (how to think about it)
Typical cost ranges for EHR software development:
| Scope | Estimated cost | Timeline |
| Basic EHR/EMR (single specialty, limited integrations) | $40,000–$150,000 | 4–8 months |
| Mid-complexity EHR (multi-specialty, lab/pharmacy integrations, patient portal) | $150,000–$500,000 | 8–14 months |
| Enterprise EHR (multi-facility, full interoperability, analytics, CDS) | $500,000–$2,000,000+ | 14–24+ months |
These ranges depend heavily on integration complexity, data migration scope, compliance requirements, and team location. According to KLAS Research, EHR implementation costs frequently exceed initial estimates by 20–30% due to underestimated integration and data migration efforts. Offshore EHR developers (e.g., Vietnam-based teams at $28–$46/hour) can reduce costs by 40–60% compared to US-based teams, while maintaining quality when properly governed.
Cost breakdown components:
- Engineering, QA experts, compliance testing, infrastructure costs, third-party integrations, licensing fees (if hybrid), training
- Hidden costs: integration requirements growth, data cleansing for migration, downtime contingencies, security audits, support staffing
- Ongoing operational costs: monitoring, patching, incident response, annual maintenance and support costs (typically 15–20% of initial build cost per year)
What I’d do in your position:
Build a business case development doc with:
- Top 3 operational pain points (measurable)
- Target improvements (billing accuracy, reduced rework, faster throughput)
- Implementation risks and mitigations
- TCO over 3–5 years (build vs buy vs hybrid)
Decision checklist (use this in procurement and executive reviews)
Strategy & scope
1. What’s our non-negotiable scope (must-have workflows) vs phase 2?
2. Are we building EHR, EMR, or a hybrid around existing systems?
Compliance & risk
3. Which regulations apply (HIPAA, GDPR, PDPA, APPs) and where will data be stored?
4. Do we have defined access control, audit trails, encryption, and breach processes?
Interoperability
5. Which integrations are required at go-live (labs, imaging, pharmacy, payers)?
6. Are we using HL7 FHIR and do we need SMART on FHIR app integration?
Usability & adoption
7. Have clinicians validated prototypes with realistic scenarios?
8. Do we have a training and change management plan?
Operational readiness
9. What are uptime targets, RPO/RTO, and downtime procedures?
10. Do we have monitoring, incident response, and support staffing?
Future trends in EHR and EMR software development (what’s real vs what’s hype)
AI-assisted clinical documentation (real, but governance-heavy)
Generative AI is already reducing documentation burden in EHR systems. According to a Stanford Medicine study, AI-powered ambient documentation tools can reduce clinician documentation time by up to 50%. However, you must design for:
- clinician review/attestation (the human must verify AI-generated notes)
- traceability (what was suggested vs what the clinician accepted)
- data privacy and model boundaries (PHI must not leak to external AI services without proper BAAs)
Predictive analytics and population health management
Value depends on data quality, coding consistency, and governance; otherwise, you get false signals. Organizations with clean, structured EHR data can use predictive models for readmission risk, chronic disease management, and resource allocation, but only if the underlying data governance is in place first.
Patient-centric, interoperable ecosystems
FHIR + SMART patterns continue to expand app ecosystems and patient access models.
Regulatory evolution (especially around CDS)
In the US, the FDA provides guidance clarifying which CDS functions may be excluded from device definition and which may remain regulated, which is important if your EHR includes advanced CDS or patient-facing decision logic.
Conclusion
EHR software development and EMR software development work best when you treat them as clinical workflow and risk-management programs, not typical software builds. The highest-impact teams start by mapping a few high-volume workflows, validating them with clinicians, and designing interoperability(HL7 FHIR), security, and auditability from day one.
Custom build, ready-made platform, or hybrid, the real differentiators are the same: usability, integration reliability, data governance, and a realistic total cost of ownership (TCO) model that accounts for support and compliance. If you focus on measurable outcomes, clinical efficiency, billing accuracy, and patient satisfaction, you’ll invest in an EHR system that strengthens operations instead of creating long-term complexity.
Contact Saigon Technology for a free EHR software development consultation, no commitment, no sales pressure, just a practical conversation about your requirements. With 14 years of experience, 400+ engineers, ISO 27001/ISO 9001 certifications, and proven delivery across the US, Australia, Europe, and Singapore, including healthcare platforms managing millions of medical records, we can help you evaluate the right approach. Start with a 2-week risk-free trial of our development team to see the quality firsthand.
FAQ
1. What’s the difference between EHR software development and EMR software development?
In practice, they overlap. EMR software development often focuses on internal charting and practice workflows, while EHR software development more often emphasizes interoperability and continuity of care. Define the difference in your requirements, not by vendor terminology.
2. How long does EHR software development take?
For a meaningful first release, many teams need 6–12 months, depending on integrations, data migration, and compliance scope. Full replacement programs can take longer. The biggest drivers are integration complexity and stakeholder requirements gathering.
3. What standards should our EHR support?
At a minimum, plan for HL7 FHIR for modern API interoperability. If you need third-party apps to launch inside the EHR securely, consider SMART on FHIR.
4. What compliance requirements matter most across the US, EU, AU, and Singapore?
- US: HIPAA Security Rule safeguards (admin/physical/technical).
- EU: GDPR, including stricter handling of health data.
- Singapore: PDPA obligations and PDPC healthcare guidance, including transfer limitation and breach notification.
- Australia: APPs and health privacy guidance.
5. How do we estimate the total cost of ownership (TCO)?
Include:
- build cost (engineering + QA + product + security)
- integration development and interface monitoring
- infrastructure + environments
- compliance audits and security testing
- training, go-live support, ongoing maintenance
Then compare build vs buy vs hybrid over 3–5 years.
6. How do we choose between an EHR software development company and building in-house?
If speed and compliance maturity are concerns, an experienced EHR software development company can reduce delivery risk, but only if you retain ownership of requirements, governance, and clinical validation. In-house teams offer tighter control long term but require a strong security/compliance operating model.
7. What should we ask EMR software developers in an RFP?
Ask about:
- prior healthcare integrations (HL7 v2, FHIR, imaging, labs)
- security implementation process (MFA, RBAC, encryption, audit trails)
- usability testing approach with clinicians
- downtime procedures and monitoring
- experience with multi-region regulatory requirements
8. Does clinical decision support make our EHR a regulated medical device in the US?
Not always. FDA guidance clarifies how certain CDS functions may be excluded from device definition and when FDA oversight may apply; this depends on the function and intended use. Get regulatory counsel if you’re building advanced CDS.
9. How much does it cost to develop EHR software?
Costs vary significantly by scope. A basic single-specialty EHR or EMR typically costs $40,000–$150,000 with a 4–8 month timeline. Mid-complexity systems with lab/pharmacy integrations and patient portals range from $150,000–$500,000 (8–14 months). Enterprise-grade EHR systems with full interoperability, analytics, and clinical decision support can exceed $500,000–$2,000,000+ over 14–24 months. Offshore EHR developers can reduce costs by 40–60% compared to US-based teams.
10. What is the best technology stack for EHR development?
There’s no single “best” stack, but most successful EHR systems use a modern frontend framework (React, Angular, or Vue), a proven backend (Node.js, .NET Core, Java/Spring Boot, or Python/FastAPI), a relational database (PostgreSQL or SQL Server), and a FHIR-compliant integration layer. Cloud infrastructure (AWS, Azure, or GCP) with HIPAA BAA support is standard. The right choice depends on your team’s expertise, integration requirements, and compliance needs.
11. How do I build an EHR system from scratch?
Start with a thin-slice prototype: map one end-to-end clinical workflow (e.g., patient intake → visit note → lab order → result review → billing handoff). Validate it with clinicians before scaling. Key steps: (1) discovery and requirements analysis with clinical stakeholders, (2) UX/UI design tested with real users, (3) architecture decisions including FHIR interoperability and HIPAA compliance, (4) iterative development with security testing at every sprint, (5) phased deployment with clinician training and go-live support. Most teams need 6–12 months for a meaningful first release.
Author (experience & perspective)
Phuc (Cris) Tran – Author: Healthcare Software Development Consultant at Saigon Technology, specializing in EHR/EMR platforms, interoperability (HL7 FHIR, SMART on FHIR), and security by design. Cris has contributed to EHR software development programs across the US, Australia, and Southeast Asia, working with clinical stakeholders to design systems that balance compliance, usability, and long-term maintainability.
How this guide was written: Based on common delivery patterns and risks seen across EHR and EMR modernization programs at Saigon Technology and in the broader healthcare IT industry, aligned to publicly available regulatory and standards references cited above.
Sources (selected)
- HHS: Summary of the HIPAA Security Rule
- NIST: SP 800-66 Rev. 2 (HIPAA Security Rule implementation guidance)
- HL7: FHIR Overview
- SMART Health IT: SMART on FHIR API overview
- EU GDPR: Article 9 (special category data, including health data)
- Singapore PDPC: PDPA overview + Healthcare sector advisory guidelines
- OAIC (Australia): Australian Privacy Principles + health privacy guide
- FDA: Clinical Decision Support Software guidance